According to the World Health Organization Trusted Source, most individuals will get a headache at some point in their lives. While they can be unpleasant and debilitating at times, the majority of them can be managed with over-the-counter pain relievers and will go away within a few hours. Repeated bouts or specific sorts of headaches, on the other hand, might indicate something more serious. Many of us have experienced the throbbing, unpleasant, and distracting agony of a headache in some form. Headaches come in a variety of forms.
Everyone gets a headache at some point in their lives. Although headaches are described as pain “in any region of the head,” the pain’s source, duration, and intensity vary depending on the kind. In certain situations, a headache need medical attention right away. If you have any of the following symptoms in addition to your headache, get medical help right once. If your headache isn’t too bad, keep reading to find out how to recognise the sort of headache you’re having and what you can do to relieve your symptoms.
What Are The Causes Of Headaches?
A headache is caused by a complex interplay of messages between your brain, blood vessels, and surrounding nerves. Pain signals are sent to your brain by specific nerves in your blood vessels and head muscles. However, it is unclear how these signals are activated in the first place.
Is It True That Headaches Run on Families?
Migraines, in particular, have a tendency to run in families. Migraine sufferers are more likely to have at least one parent who also suffers from the condition. In fact, children whose parents suffer from migraines are four times more likely to suffer from them themselves. Headaches can also be induced by elements that are common in a family’s surroundings, such as:
- Caffeine, alcohol, fermented foods, chocolate, and cheese are some of the foods or components to avoid.
- Allergen exposure is a term used to describe the process of becoming exposed to allergens.
- Tobacco smoke that has been passed down from one generation to the next
- Strong smells from perfumes or household chemicals.
What Can I Do To Avoid Getting a Headache?
Finding out what causes headaches is crucial to preventing them. Triggers are unique to each individual; what gives you a headache may not bother others. You can avoid or limit your triggers after you’ve identified them. You may, for example, discover that strong fragrances irritate you. Avoiding fragrances and scented items can significantly reduce the number of headaches you get. Other typical causes include irritable meals, little sleep, and bad posture.
Many others, on the other hand, are either unable to avoid or recognise triggers. In such cases, a more tailored interdisciplinary treatment involving a headache specialist is frequently required.
Is It Possible To Get Rid Of Headaches or Migraines?
Headaches can be relieved by treating health issues that cause them, such as high blood pressure. There have been a few recent breakthroughs in our knowledge of what causes headaches. Although we are closer to a solution than we have ever been, there is still no cure for primary headaches. The goal of treatment is to alleviate symptoms while also preventing future occurrences.
When Should You Go To The Doctor?
Episodic headaches usually go gone in 48 hours or less. If you experience a headache that lasts longer than two days or becomes more intense, you should seek medical help. You may have a chronic headache problem if you get headaches for more than 15 days per month for more than three months. Even if you can manage the discomfort with aspirin or ibuprofen, you should see your doctor to find out what’s wrong. Headaches can be a sign of more serious health problems, and some of them require more than over-the-counter medicines and home cures to address.
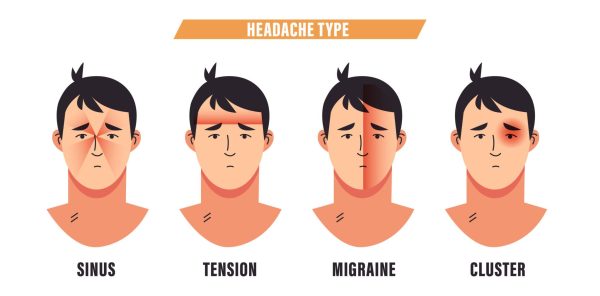
Different Types of Headaches
Headaches are common, but they’re not always the same. Here’s what you need to know about different types of headaches.
1. Tension Headaches
A dull, painful sensation may be felt all over your head if you have a tension headache. It isn’t throbbing at all. Tenderness or sensitivity in the muscles of the neck, forehead, scalp, or shoulders is also possible. Tension headaches may affect anybody, and they’re frequently brought on by stress. An over-the-counter (OTC) pain medication may be all you need to alleviate your symptoms on occasion. This includes the following:
If over-the-counter medicines don’t work, your doctor may prescribe a prescription medication. Indomethacin, meloxicam (MOBIC), and ketorolac are among examples.
When a tension headache becomes persistent, a different approach to addressing the underlying headache trigger may be advised.
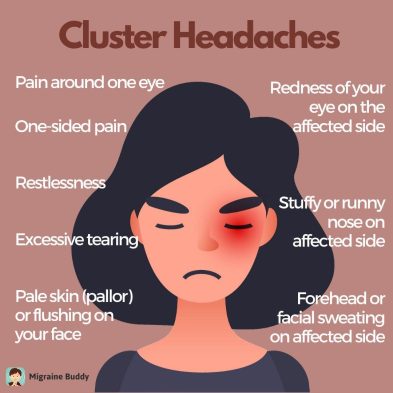
2. Cluster Headaches
Cluster headaches cause excruciating searing and piercing agony. At a time, they appear around or behind one eye or on one side of the face. On the side of the head that is impacted by the headache, edoema, redness, flushing, and sweating might develop. On the same side as the headache, nasal congestion and eye tears are common.
This is the first in a sequence of headaches. Each headache might last anywhere from 15 minutes to three hours. During a cluster, most patients get one to four headaches each day, generally at the same time each day. After one headache subsides, another will appear soon after. Cluster headaches can occur on a daily basis for months at a time. Individuals are symptom-free in the months between clusters. In the spring and fall, cluster headaches are more prevalent. Men are also three times more likely to have them.
Doctors don’t know what causes cluster headaches, but they do know how to treat the symptoms effectively. Your doctor may prescribe oxygen therapy, sumatriptan (Imitrex), or a topical anaesthetic (lidocaine) to relieve discomfort. Your doctor will work with you to establish a preventive strategy after a diagnosis has been made. Corticosteroids, melatonin, topiramate (Topamax), and calcium channel blockers can help you get rid of your cluster headaches.
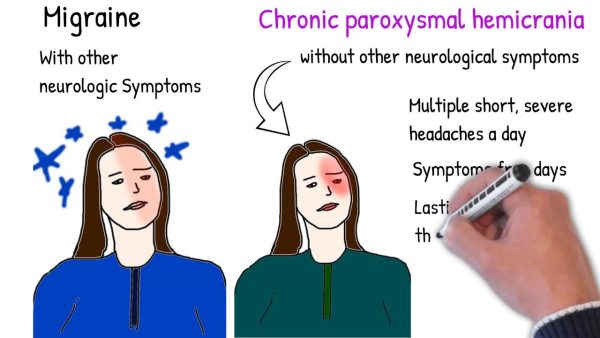
3. Migraine
Migraine pain is a pulsating sensation that originates deep within your skull. This discomfort might persist for many days. The headache severely hampers your ability to carry out your regular routine. Migraines are throbbing headaches that are generally one-sided. Migraine sufferers are frequently light and sound sensitive. Nausea and vomiting are common side effects. Visual problems might precede migraine in some cases. Before the headache begins, around one out of every five persons may experience these symptoms. It’s called an aura, and it may make you see things like:
Tingling on one side of your face or in one arm, as well as difficulty speaking, are all signs of auras. However, because the symptoms of a stroke might be similar to those of a migraine, if any of these symptoms are new to you, you should seek medical help right once. Migraine episodes can run in families, or they might be linked to other nervous system disorders. Women are three times as likely than males to suffer from migraines. Migraines are more common in those who have post-traumatic stress disorder.
Sleep disturbance, dehydration, missing meals, certain foods, hormone changes, and chemical exposure are all frequent migraine causes. If over-the-counter pain medications don’t help your migraine discomfort, your doctor may prescribe triptans. Triptans are medications that reduce inflammation and alter blood flow in the brain. Nasal sprays, tablets, and injections are all options.
If you get debilitating headaches more than three times per month, moderately debilitating headaches four times per month, or any headaches at least six times per month, talk to your doctor about taking a daily prescription to prevent your headaches.
Preventative medicines are largely underutilized, according to research. Only 3 to 13% of migraine sufferers use preventative medicine, despite the fact that up to 38% of them require it. Migraine prevention substantially enhances one’s quality of life and productivity.
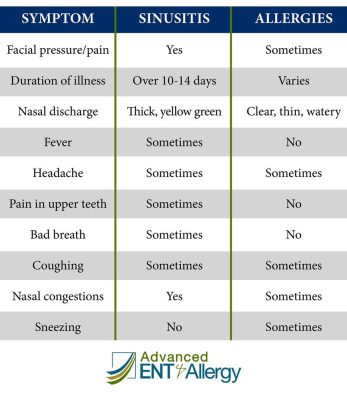
4. Allergy or Sinus Headaches
An allergic response might cause headaches in certain people. The pain from these headaches is usually concentrated in the area around your sinuses and at the front of your head. Sinus headaches are sometimes mistaken as migraine headaches. Up to 90% of so-called “sinus headaches” are actually migraines. These headaches are more common in people who suffer from seasonal allergies or sinusitis.
The mucus that builds up and creates sinus pressure is thinned out to relieve sinus headaches. Nasal steroid sprays, over-the-counter decongestants such phenylephrine (Sudafed PE), and antihistamines like cetirizine (Zyrtec D Allergy + Congestion) can assist. Sinus headaches are also a sign of a sinus infection. Antibiotics may be prescribed in certain situations to remove the infection and ease your headache and other symptoms.
5. Hormone Headaches
Hormonal changes are often associated with headaches in women. Estrogen levels are affected by menstruation, birth control pills, and pregnancy, all of which can produce a headache. Menstrual migraine refers to migraines that are especially linked to the menstrual cycle. They can happen before, during, or after menstruation, as well as during ovulation.
This discomfort can be managed with over-the-counter pain medicines like naproxen (Aleve) or prescription drugs like frovatripan (Frova). Because it’s believed that around 60% of women with migraine also suffer menstrual migraine, different treatments might help reduce total migraines per month. Migraine headaches can be prevented using relaxation methods, yoga, acupuncture, and a changed diet.
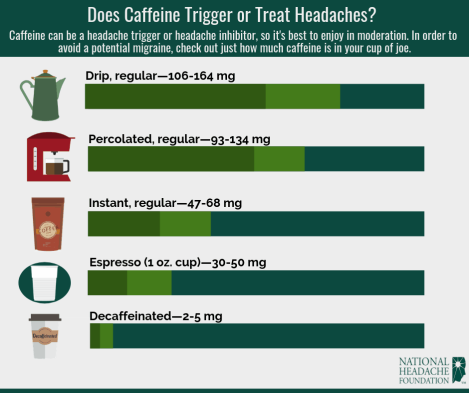
6. Caffeine Headaches
Caffeine has an effect on cerebral blood flow. Caffeine overdose, as well as stopping caffeine “cold turkey,” can cause headaches. Caffeine users who suffer from migraines frequently are at risk of causing a headache.
You could develop a headache if you don’t receive your caffeine fix if you’re used to exposing your brain to a specific quantity of caffeine, a stimulant, each day. This might be due to the fact that caffeine alters brain chemistry, and withdrawal from it can produce a headache. Not everyone who reduces their coffee intake will suffer withdrawal symptoms. Keeping your caffeine intake at a consistent, acceptable amount ” or completely eliminating it ” might help you avoid headaches.
7. Exertion Headaches
Exertion headaches occur immediately following periods of vigorous physical exercise. Exercising, jogging, and sexual activity are all frequent causes of exertion headaches. These activities are considered to increase blood flow to your skull, resulting in a pounding headache on both sides of your head.
An exercise headache should not last more than a few hours. This sort of headache generally passes in a matter of minutes or hours. Analgesics like aspirin and ibuprofen (Advil) should help you feel better. Make an appointment with your doctor if you experience exertion headaches. They might be a symptom of a dangerous underlying pharmaceutical problem in rare situations.
8. Hypertension Headaches
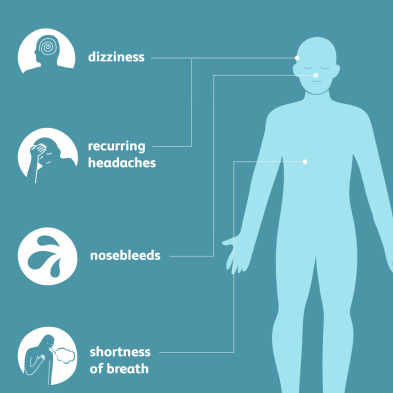
High blood pressure can induce a headache, and this type of headache should be treated as an emergency. When your blood pressure rises to dangerously high levels, this happens. A hypertension headache usually affects both sides of your head and is exacerbated by physical exertion. It has a pulsing feel to it. Possible symptoms include changes in eyesight, numbness or tingling, nosebleeds, chest discomfort, or shortness of breath.
If you suspect you’re having a hypertension headache, you should visit a doctor right away. If you’re taking medication for high blood pressure, you’re more prone to have this sort of headache. These sorts of headaches usually go after your blood pressure is under control. They shouldn’t happen again as long as your blood pressure is under control.
9. Rebound Headaches
Rebound headaches, also known as drug overuse headaches, can be dull and tension-like or more severely painful, similar to a migraine. If you use over-the-counter pain medications often, you may be more vulnerable to this sort of headache. Overuse of these medicines leads to an increase in headaches rather than a decrease in headaches.
When OTC medicines such acetaminophen, ibuprofen, aspirin, and naproxen are taken for more than 15 days in a month, rebound headaches are more likely to develop. They’re also more prevalent with caffeine-containing medicines.
The only way to get rid of rebound headaches is to wean yourself off of the pain medication you’ve been using. Although the discomfort may initially intensify, it should diminish entirely within a few days. Taking a preventative daily drug that does not induce rebound headaches and prevents migraines from forming in the first place is a smart strategy to avoid medication overuse headaches.
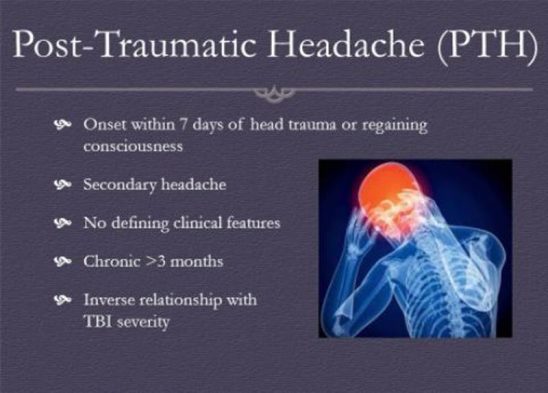
10. Post-Traumatic Headaches
Any form of head injury might result in post-traumatic headaches. These headaches are similar to migraines or tension headaches, and they can continue anywhere from 6 to 12 months following an accident. They have the potential to become chronic. Triptans, sumatriptan (Imitrex), beta-blockers, and amitriptyline are frequently given to treat these headaches.
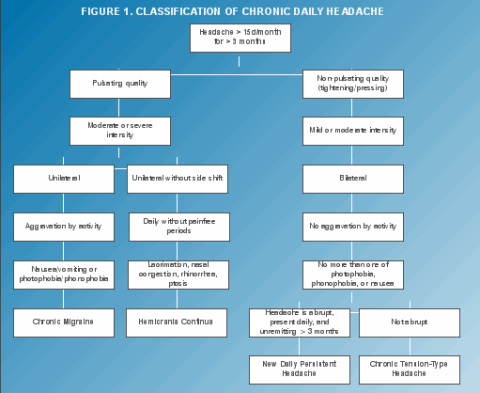
11. Chronic Daily Headaches
For more than three months, you’ve had this sort of headache 15 days or more per month. Some are only a few words long. Others go on for more than four hours. It’s generally one of four major headache types:
- Migraine attacks on a regular basis.
- Tension headaches are common.
- A new everyday chronic headache has appeared.
- Hemicrania persists.
12. Exercise Headaches
The muscles in your head, neck, and scalp require more blood while you’re active. To supply them, your blood vessels expand. A pulsating ache on both sides of your head might persist anywhere from 5 minutes to 48 hours as a result of this condition. It generally happens while you’re doing something vigorous or shortly thereafter, whether it’s exercise or intercourse.
13. Hemicrania Continua
Hemicrania continua is a type of persistent headache that affects the same side of your face and head virtually all of the time. Other signs and symptoms include:
- Pain that varies in severity
- Eyes that are red or teary
- A stuffy or runny nose
- Eyelid droops
- IRIS contract
- Indomethacin, a pain reliever, is effective
- Physical exercise makes the discomfort worse
- Drinking alcohol makes the discomfort worse
- Vomiting and nausea
- Light and sound sensitivity
14. New Daily Persistent Headaches (Ndph)
These can appear out of nowhere and last for three months or longer. Many folks recall the exact date when their suffering began. Doctors are baffled as to why this sort of headache develops. It can strike after an infection, flu-like sickness, surgery, or a stressful event for certain people. The discomfort is usually mild, although it can be severe in certain cases. It’s also notoriously difficult to cure. Symptoms might range from mild to severe. Some of them are similar to stress headaches. Others get migraine symptoms including nausea or light sensitivity.
If your headache persists or becomes severe, contact your doctor.
15. Ice Pick Headaches
These severe, stabbing headaches generally last barely a few seconds. At most, they occur a few times every day. See a doctor if you have one. Ice pick headaches can be a standalone ailment or a sign of something more serious.
16. Spinal Headaches
Talk to your doctor if you experience a headache after a spinal tap, spinal block, or epidural. Because these treatments entail penetrating the membrane that covers your spinal cord, your doctor may refer to it as a puncture headache. A headache might occur if spinal fluid escapes through the puncture site. This is commonly referred to as “the worst headache of your life.” It appears out of nowhere and soon peaks. Thunderclap headaches can be caused by a variety of factors, including:
- Tear, rupture, or obstruction of a blood vessel
- Injuries to the head
- A burst blood artery in your brain causes a hemorrhagic stroke
- A clogged blood artery in your brain causes an ischemic stroke
- Blood arteries around the brain are narrowed
- Blood vessels that are inflamed
- Changes in blood pressure during late pregnancy
A sudden new headache should be taken carefully. It’s frequently the only indication you have of a major condition.
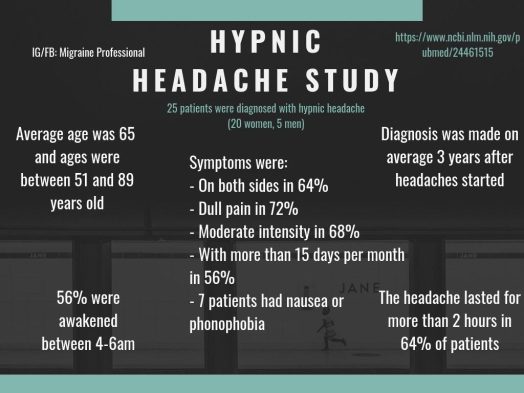
17. Hypnic Headaches
A hypnic headache is an uncommon disease that generally strikes in a person’s 50s, although it can strike at any age. They’re also known as “alarm clock” headaches since they wake individuals up in the middle of the night. A hypnic headache is characterized by mild to severe throbbing pain on both sides of the head. Other symptoms include nausea and sensitivity to light and sound, and it can last up to 3 hours.
Each week, people may be subjected to many attacks. There is no known cause for hypnic headaches, and there are no recognized triggers. Despite the fact that hypnic headaches are safe, an older person who has a new type of headache for the first time should consult a physician. Migraine and cluster headaches must be ruled out as well. Caffeine is the most popular therapy, which may be given as pills or as cups of coffee before night. Indomethacin, melatonin, and lithium are some of the other medications available.
18. Medication-Overuse Headaches
The most frequent kind of secondary headache is medication-overuse headache (MOH), often known as a rebound headache. Regular or daily headaches characterise a MOH with symptoms that are comparable to tension or migraine headaches. These headaches react to medicines at first, but they return after a while. Taking painkillers for more than 15 days in a month might cause MOH. MOH can be caused by a variety of medications, including:
- Opioids
- Acetaminophen
- Sumatriptan, for example, is a kind of triptan
- Aspirin and ibuprofen are examples of nonsteroidal anti-inflammatory drugs (NSAIDs)
Despite taking these medicines as prescribed, a MOH might still occur. A MOH, on the other hand, appears to develop mostly in persons who are using analgesics for the treatment of a headache. The only way to get rid of MOH is to stop using the headache medication. Anyone who wants to quit taking medicine should do so under the guidance of a doctor. The doctor will be able to assist in the creation of a plan and may be able to prescribe additional medications to help with the withdrawal process. After quitting the medication, symptoms are likely to increase before improving. Within 10 days, the headaches should be gone.
Additional withdrawal symptoms generally subside after seven days, although they might last up to three weeks. These are some of them:
- Vomiting and nausea
- A faster heartbeat
- Sleep disruption
- Anxiety, restlessness, and anxiousness are all symptoms of restlessness
Within two months, the majority of patients return to their previous headache pattern. After that, you should be able to resume using pain relievers.
19. Head-Injury Headaches
Minor bumps and knocks to the head and neck are quite common and typically cause no concern. A headache may occur immediately or shortly thereafter. These are commonly confused with migraines or tension headaches and are generally treated with over-the-counter pain relievers. Anyone who has headaches that are chronic or intensifying should consult a doctor. Always contact an ambulance if someone has suffered a major head injury or if they are experiencing any of the following symptoms after a head injury:
- Unconsciousness
- Seizures
- Vomiting
- Loss of memory
- Confusion
- Difficulties with vision or hearing
20. Menstrual Headaches
Changes in hormone levels are frequently linked to headaches. Migraine is commonly associated with menstruation in women, owing to natural fluctuations in oestrogen levels. Menstrual migraines occur in the days leading up to or during a period, as well as during ovulation. The symptoms are similar to those of a migraine without aura, although they might persist longer and be more incapacitating.
Hormone headaches can also be brought on by:
- Contraceptive pills
- Menopause is a term used to describe a period of time
- Pregnancy
Menstrual headaches are treated in the same way as migraines without aura are treated.
21. Hormonal Therapy
- Taking a triptan or an NSAID around menstruation time
- Other methods of oral contraception, such as skipping the pill-free period
- Hormone replacement treatment for postmenopausal women
22. Hangover Headaches
Overindulging in alcoholic beverages might result in a throbbing headache the next morning or even later that day. Movement aggravates these migraine-like headaches, which generally affect both sides of the brain. Nausea and light sensitivity are common side effects of a hangover headache. Although there are no treatments for hangovers, they can be alleviated by drinking plenty of water and eating sweet foods. OTC pain relievers may assist to relieve or eliminate headache discomfort.
Hangover symptoms usually subside after 72 hours.
You may minimize your chances of developing a hangover by:
- Consuming alcohol in moderation
- Avoiding consuming alcohol on an empty stomach
- Between alcoholic beverages and before going to bed, drink plenty of water.